Abstract
Background
Resection of breast cancer liver metastases (BCLM) combined with systemic treatment is increasingly accepted as a therapeutic option; however, the potential benefit of repeat hepatectomy for recurrent BCLM is unknown.
Methods
All consecutive female patients who underwent liver resection for BCLM at our center between January 1985 and December 2012 were included. Patients who had a single hepatectomy (N = 120) were compared with those who also underwent repeat hepatectomy (N = 19). Patients were selected for repeat hepatectomy based on operability and disease control. Prognostic factors of survival after repeat hepatectomy were determined.
Results
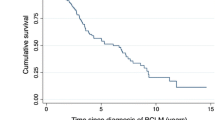
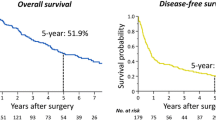
Median overall survival since first hepatectomy was 35 months, with a 3- and 5-year survival rate of 50 and 38 %, respectively. Overall survival following repeat hepatectomy was 64 and 46 % at 3 and 5 years, respectively. From the time of first hepatectomy, patients who underwent repeat hepatectomy had a better survival than those who had only one hepatectomy (95 and 84 vs. 50 and 38 % at 3 and 5 years, respectively) (p = 0.002). Median survival was 35 and 100 months, respectively, and median survival since the diagnosis of BCLM was 51 and 112 months in the single and repeat hepatectomy groups, respectively. Since the time of diagnosis, overall 3-, 5-, and 7-year survival rates were 75, 57, and 44 %, respectively, for all 139 patients. Improved overall survival after repeat hepatectomy was related to a time interval between breast cancer diagnosis and first hepatectomy of >2 years, a limited hepatectomy, solitary liver metastasis, positive progesterone receptor status, and chemotherapy following repeat hepatectomy. Patients with single BCLM at first hepatectomy had a 3- and 5-year overall survival rate of 76 and 76 % compared with 51 and 17 % in patients with multiple metastases (p = 0.023).
Conclusion
In selected patients with BCLM, repeat hepatectomy for liver recurrence combined with systemic treatment provided survival rates comparable to those after first hepatectomy.


Similar content being viewed by others
References
Jemal A, Bray F, Center MM, et al. Global cancer statistics. CA Cancer J Clin. 2011;61(2):69–90.
Siegel R, Naishadham D, Jemal A. Cancer statistics, 2013. CA Cancer J Clin. 2013;63(1):11–30.
Miller KD, Sledge GW Jr. The role of chemotherapy for metastatic breast cancer. Hematol Oncol Clin North Am. 1999;13(2):415–34.
Schuetz F, Diel IJ, Pueschel M, et al. Reduced incidence of distant metastases and lower mortality in 1072 patients with breast cancer with a history of hormone replacement therapy. Am J Obstet Gynecol. 2007;196(4):342.e1–9.
Kennecke H, Yerushalmi R, Woods R, et al. Metastatic behavior of breast cancer subtypes. J Clin Oncol. 2010;28(20):3271–7.
Pogoda K, Niwinska A, Murawska M, et al. Analysis of pattern, time and risk factors influencing recurrence in triple-negative breast cancer patients. Med Oncol. 2013;30(1):388.
Berman AT, Thukral AD, Hwang WT, et al. Incidence and patterns of distant metastases for patients with early-stage breast cancer after breast conservation treatment. Clin Breast Cancer. 2013;13(2):88–94.
Follana P, Barriere J, Chamorey E, et al. Prognostic factors in 401 elderly women with metastatic breast cancer. Oncology. 2014;86(3):143–51.
Sugihara K, Uetake H. Therapeutic strategies for hepatic metastasis of colorectal cancer: overview. J Hepatobiliary Pancreat Sci. 2012;19(5):523–7.
Fedorowicz Z, Lodge M, Al-asfoor A, et al. Resection versus no intervention or other surgical interventions for colorectal cancer liver metastases. New York: Wiley; 2008.
Chua TC, Saxena A, Liauw W, et al. Hepatic resection for metastatic breast cancer: a systematic review. Eur J Cancer. 2011;47(15):2282–90.
Wicherts DA, de Haas RJ, Salloum C, et al. Repeat hepatectomy for recurrent colorectal metastases. Br J Surg. 2013;100(6):808–18.
Adam R, Aloia T, Krissat J, et al. Is liver resection justified for patients with hepatic metastases from breast cancer? Ann Surg. 2006;244(6):897–907. discussion 907–8.
Caralt M, Bilbao I, Cortes J, et al. Hepatic resection for liver metastases as part of the “oncosurgical” treatment of metastatic breast cancer. Ann Surg Oncol. 2008;15(10):2804–10.
Kollmar O, Moussavian MR, Richter S, et al. Surgery of liver metastasis in gynecological cancer: indication and results. Onkologie. 2008;31(7):375–9.
Lubrano J, Roman H, Tarrab S, et al. Liver resection for breast cancer metastasis: does it improve survival? Surg Today. 2008;38(4):293–9.
Thelen A, Benckert C, Jonas S, et al. Liver resection for metastases from breast cancer. J Surg Oncol. 2008;97(1):25–9.
Hoffmann K, Franz C, Hinz U, et al. Liver resection for multimodal treatment of breast cancer metastases: identification of prognostic factors. Ann Surg Oncol. 2010;17(6):1546–54.
Rubino A, Doci R, Foteuh JC, et al. Hepatic metastases from breast cancer. Updates Surg. 2010;62(3–4):143–8.
Cassera MA, Hammill CW, Ujiki MB, et al. Surgical management of breast cancer liver metastases. HPB. 2011;13(4):272–8.
Abbott DE, Brouquet A, Mittendorf EA, et al. Resection of liver metastases from breast cancer: estrogen receptor status and response to chemotherapy before metastasectomy define outcome. Surgery. 2012;151(5):710–6.
Duan XF, Dong NN, Zhang T, et al. Comparison of surgical outcomes in patients with colorectal liver metastases versus non-colorectal liver metastases: a Chinese experience. Hepatol Res. 2012;42(3):296–303.
Groeschl RT, Nachmany I, Steel JL, et al. Hepatectomy for noncolorectal non-neuroendocrine metastatic cancer: a multi-institutional analysis. J Am Coll Surg. 2012;214(5):769–77.
van Walsum GA, de Ridder JA, Verhoef C, et al. Resection of liver metastases in patients with breast cancer: survival and prognostic factors. Eur J Surg Oncol. 2012;38(10):910–7.
Dittmar Y, Altendorf-Hofmann A, Schule S, et al. Liver resection in selected patients with metastatic breast cancer: a single-centre analysis and review of literature. J Cancer Res Clin Oncol. 2013;139(8):1317–25.
Kostov DV, Kobakov GL, Yankov DV. Prognostic factors related to surgical outcome of liver metastases of breast cancer. J Breast Cancer. 2013;16(2):184–92.
Polistina F, Costantin G, Febbraro A, et al. Aggressive treatment for hepatic metastases from breast cancer: results from a single center. World J Surg. 2013;37(6):1322–32.
Kim JY, Park JS, Lee SA, et al. Does liver resection provide long-term survival benefits for breast cancer patients with liver metastasis? A single hospital experience. Yonsei Med J. 2014;55(3):558–62.
Weinrich M, Weiss C, Schuld J, et al. Liver resections of isolated liver metastasis in breast cancer: results and possible prognostic factors. HPB Surg. 2014;2014:893829.
Couinaud C. Variations of the right bile ducts. The futility of complete anatomical classifications [in French]. Chirurgie 1993;119(6–7):354–6.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240(2):205–13.
Abuzallouf S, Motawy M, Thotathil Z. Baseline staging of newly diagnosed breast cancer: Kuwait cancer control center experience. Med Princ Pract. 2007;16(1):22–4.
Rubbia-Brandt L, Giostra E, Brezault C, et al. Importance of histological tumor response assessment in predicting the outcome in patients with colorectal liver metastases treated with neo-adjuvant chemotherapy followed by liver surgery. Ann Oncol. 2007;18(2):299–304.
Blazer DG 3rd, Kishi Y, Maru DM, et al. Pathologic response to preoperative chemotherapy: a new outcome end point after resection of hepatic colorectal metastases. J Clin Oncol. 2008;26(33):5344–51.
Acknowledgement
The Netherlands Organization for Scientific Research (NWO) provided funding for a research fellow.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ruiz, A., Castro-Benitez, C., Sebagh, M. et al. Repeat Hepatectomy for Breast Cancer Liver Metastases. Ann Surg Oncol 22 (Suppl 3), 1057–1066 (2015). https://doi.org/10.1245/s10434-015-4785-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-015-4785-8