Abstract
Background
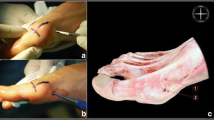
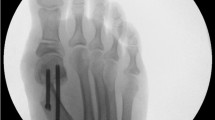
In the last decade, interests in minimal incision surgery have been growing. Theoretically, this kind of procedure could decrease time to recovery and rehabilitation, with a reduction in morbidity. The present study assessed clinical and radiological outcomes and complications of percutaneous surgery for mild-to-moderate hallux valgus using Reverdin–Isham and Akin osteotomies without fixation after 60 months of follow-up.
Methods
A series of 48 patients (57 cases) with medium-to-moderate hallux valgus underwent the same percutaneous surgery, between 2003 and 2011. Data collection involved preoperative dorsal flexion, plantar flexion, M1P1, M1M2, DMAA angles, AOFAS scale score, and subjective satisfaction.
Results
AOFAS scale score rose from a preoperative median of 55.9–89.2/100 postoperatively (p < 0.001); 51 surgical procedures (89.5%) were considered as satisfactory or very satisfactory by patients at the end of follow-up. Hallux valgus and distal metatarsal articular angle (DMAA) were significantly reduced (29.3° and 14.1°–15.4° and 7.7°, p < 0.001, respectively). There was a significant increase in MTPJ 1 stiffness (p < 0.001).
Discussion
Percutaneous correction by Reverdin–Isham and Akin osteotomies seems to be effective in isolated medium-to-moderate hallux valgus. Stiffness observed is comparable to other percutaneous and open procedures but needs to be compared in a randomized controlled clinical trial to extra-articular percutaneous procedures without capsule detachment in association with an internal fixation which allows an early mobilization.
Level of clinical evidence
IV.



Similar content being viewed by others
References
Bauer T, Biau D, Lortat-Jacob A, Hardy P (2010) Percutaneous hallux valgus correction using the Reverdin–Isham osteotomy. Orthop Traumatol Surg Res 96(4):407–416
Brogan K, Voller T, Gee C, Borbely T, Palmer S (2014) Third-generation minimally invasive correction of hallux valgus: technique and early outcomes. Int Orthop 38(10):2115–2121
Isham SA (1991) The Reverdin–Isham procedure for the correction of hallux abducto valgus. A distal metatarsal osteotomy procedure. Clin Podiatr Med Surg 8(1):81–94
Magnan B, Samaila E, Viola G, Bartolozzi P (2008) Minimally invasive retrocapital osteotomy of the first metatarsal in hallux valgus deformity. Oper Orthop Traumatol 20(1):89–96
Giannini S, Faldini C, Nanni M, Di Martino A, Luciani D, Vannini F (2013) A minimally invasive technique for surgical treatment of hallux valgus: simple, effective, rapid, inexpensive (SERI). Int Orthop 37(9):1805–1813
Redfern D, Vernois J, Legré BP (2015) Percutaneous surgery of the forefoot. Clin Podiatr Med Surg 32(3):291–332
Kitaoka HB, Alexander IJ, Adelaar RS, Nunley JA, Myerson MS, Sanders M (1994) Clinical rating systems for the ankle-hindfoot, midfoot, hallux, and lesser toes. Foot Ankle Int 15(7):349–353
Ibrahim T, Beiri A, Azzabi M, Best AJ, Taylor GJ, Menon DK (2007) Reliability and validity of the subjective component of the American Orthopaedic Foot and Ankle Society clinical rating scales. J Foot Ankle Surg Off Publ Am Coll Foot Ankle Surg 46(2):65–74
Schneider W, Aigner N, Pinggera O, Knahr K (2004) Chevron osteotomy in hallux valgus. Ten-year results of 112 cases. J Bone Joint Surg Br 86(7):1016–1020
Bauer T, de Lavigne C, Biau D, De Prado M, Isham S, Laffenétre O (2009) Percutaneous hallux valgus surgery: a prospective multicenter study of 189 cases. Orthop Clin North Am 40(4):505–514
Pichierri P, Sicchiero P, Fioruzzi A, Maniscalco P (2014) Percutaneous hallux valgus surgery: strengths and weakness in our clinical experience. Acta Bio-Medica Atenei Parm 10(85 Suppl 2):121–125
Aminian A, Kelikian A, Moen T (2006) Scarf osteotomy for hallux valgus deformity: an intermediate followup of clinical and radiographic outcomes. Foot Ankle Int 27(11):883–886
Chou LB, Mann RA, Casillas MM (1998) Biplanar chevron osteotomy. Foot Ankle Int 19(9):579–584
Smith BW, Coughlin MJ (2009) Treatment of hallux valgus with increased distal metatarsal articular angle: use of double and triple osteotomies. Foot Ankle Clin 14(3):369–382
Deenik AR, Pilot P, Brandt SE, van Mameren H, Geesink RGT, Draijer WF (2007) Scarf versus chevron osteotomy in hallux valgus: a randomized controlled trial in 96 patients. Foot Ankle Int 28(5):537–541
Bock P, Kluger R, Kristen K-H, Mittlböck M, Schuh R, Trnka H-J (2015) The scarf osteotomy with minimally invasive lateral release for treatment of hallux valgus deformity: intermediate and long-term results. J Bone Joint Surg Am 97(15):1238–1245
Radl R, Leithner A, Zacherl M, Lackner U, Egger J, Windhager R (2004) The influence of personality traits on the subjective outcome of operative hallux valgus correction. Int Orthop 28(5):303–306
Sanhudo JAV (2006) Correction of moderate to severe hallux valgus deformity by a modified chevron shaft osteotomy. Foot Ankle Int 27(8):581–585
Trnka HJ, Zembsch A, Easley ME, Salzer M, Ritschl P, Myerson MS (2000) The chevron osteotomy for correction of hallux valgus. Comparison of findings after two and five years of follow-up. J Bone Joint Surg Am 82-A(10):1373–1378
Veri JP, Pirani SP, Claridge R (2001) Crescentic proximal metatarsal osteotomy for moderate to severe hallux valgus: a mean 12.2 year follow-up study. Foot Ankle Int 22(10):817–822
Fuhrmann RA, Zollinger-Kies H, Kundert H-P (2010) Mid-term results of Scarf osteotomy in hallux valgus. Int Orthop 34(7):981–989
Adam SP, Choung SC, Gu Y, O’Malley MJ (2011) Outcomes after scarf osteotomy for treatment of adult hallux valgus deformity. Clin Orthop 469(3):854–859
Díaz Fernández R (2015) Treatment of moderate and severe hallux valgus by performing percutaneous double osteotomy of the first metatarsal bone. Rev Espanola Cirugia Ortop Traumatol 59(1):52–58
Cervi S, Fioruzzi A, Bisogno L, Fioruzzi C (2014) Percutaneous surgery of allux valgus: risks and limitation in our experience. Acta Bio Med Atenei Parm 24(85 Suppl 2):107–112
Bia A, Guerra-Pinto F, Pereira BS, Corte-Real N, Oliva XM (2017) Percutaneous osteotomies in hallux valgus: a systematic review. J Foot Ankle Surg Off Publ Am Coll Foot Ankle Surg 57:123–130
Lucas y Hernandez J, Golanó P, Roshan-Zamir S, Darcel V, Chauveaux D, Laffenêtre O (2016) Treatment of moderate hallux valgus by percutaneous, extra-articular reverse-L Chevron (PERC) osteotomy. Bone Jt J 98-B(3):365–373
Bösch P, Wanke S, Legenstein R (2000) Hallux valgus correction by the method of Bösch: a new technique with a seven-to-ten-year follow-up. Foot Ankle Clin 5(3):485–498 (v–vi)
Piqué-Vidal C (2005) The effect of temperature elevation during discontinuous use of rotatory burrs in the correction of hallux valgus. J Foot Ankle Surg Off Publ Am Coll Foot Ankle Surg 44(5):336–344
Angthong C, Yoshimura I, Kanazawa K, Hagio T, Ida T, Naito M (2013) Minimally invasive distal linear metatarsal osteotomy for correction of hallux valgus: a preliminary study of clinical outcome and analytical radiographic results via a mapping system. Arch Orthop Trauma Surg 133(3):321–331
Caravelli S, Mosca M, Massimi S, Costa GG, Lo Presti M, Fuiano M et al (2017) Percutaneous treatment of hallux valgus: what’s the evidence? a systematic review. Musculoskelet Surg 102:111–117
Crespo Romero E, Peñuela Candel R, Gómez Gómez S, Arias Arias A, Arcas Ordoño A, Gálvez González J et al (2017) Percutaneous forefoot surgery for treatment of hallux valgus deformity: an intermediate prospective study. Musculoskelet Surg 101(2):167–172
Shahid MS, Lee P, Evans S, Thomas R (2012) A comparative study of bone shortening and bone loss with use of saw blades versus burr in hallux valgus surgery. Foot Ankle Surg Off J Eur Soc Foot Ankle Surg 18(3):195–197
Acknowledgements
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Severyns, M., Carret, P., Brunier-Agot, L. et al. Reverdin–Isham procedure for mild or moderate hallux valgus: clinical and radiographic outcomes. Musculoskelet Surg 103, 161–166 (2019). https://doi.org/10.1007/s12306-018-0563-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-018-0563-7