Abstract
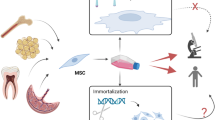
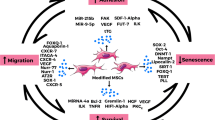
Mesenchymal stromal cells (MSCs) are promising candidates for cell-based therapies, mainly due to their unique biological properties such as multipotency, self-renewal and trophic/immunomodulatory effects. However, clinical use has proven complex due to limitations such as high variability of MSCs preparations and high number of cells required for therapies. These challenges could be circumvented with cell immortalization through genetic manipulation, and although many studies show that such approaches are safe, little is known about changes in other biological properties and functions of MSCs. In this study, we evaluated the impact of MSCs immortalization with the TERT gene on the purinergic system, which has emerged as a key modulator in a wide variety of pathophysiological conditions. After cell immortalization, MSCs-TERT displayed similar immunophenotypic profile and differentiation potential to primary MSCs. However, analysis of gene and protein expression exposed important alterations in the purinergic signaling of in vitro cultured MSCs-TERT. Immortalized cells upregulated the CD39/NTPDase1 enzyme and downregulated CD73/NT5E and adenosine deaminase (ADA), which had a direct impact on their nucleotide/nucleoside metabolism profile. Despite these alterations, adenosine did not accumulate in the extracellular space, due to increased uptake. MSCs-TERT cells presented an impaired in vitro immunosuppressive potential, as observed in an assay of co-culture with lymphocytes. Therefore, our data suggest that MSCs-TERT have altered expression of key enzymes of the extracellular nucleotides/nucleoside control, which altered key characteristics of these cells and can potentially change their therapeutic effects in tissue engineering in regenerative medicine.







Similar content being viewed by others
References
Galipeau, J., & Sensébé, L. (2018). Mesenchymal stromal cells: Clinical challenges and therapeutic opportunities. Cell Stem Cell, 22, 824–833.
da Silva, M. L., Fontes, A. M., Covas, D. T., & Caplan, A. I. (2009). Mechanisms involved in the therapeutic properties of mesenchymal stem cells. Cytokine & Growth Factor Reviews, 20, 419–427.
Uccelli, A., Moretta, L., & Pistoia, V. (2008). Mesenchymal stem cells in health and disease. Nature Reviews. Immunology, 8, 726–736.
Salem, H. K., & Thiemermann, C. (2010). Mesenchymal stromal cells: Current understanding and clinical status. Stem Cells, 28, 585–596.
Iser, I. C., Ceschini, S. M., Onzi, G. R., Bertoni, A. P. S., Lenz, G., & Wink, M. R. (2016). Conditioned medium from adipose-derived stem cells (ADSCs) promotes epithelial-to-Mesenchymal-like transition (EMT-like) in Glioma cells in vitro. Molecular Neurobiology, 53, 7184–7199.
Beckenkamp, L. R., Souza, L. E. B., Melo, F. U. F., Thomé, C. H., Magalhães, D. A. R., Palma, P. V. B., & Covas, D. T. (2018). Comparative characterization of CD271 + and CD271 − subpopulations of CD34 + human adipose-derived stromal cells. Journal of Cellular Biochemistry, 119, 3873–3884.
Onzi, G. R., Ledur, P. F., Hainzenreder, L. D., Bertoni, A. P. S., Silva, A. O., Lenz, G., & Wink, M. R. (2016). Analysis of the safety of mesenchymal stromal cells secretome for glioblastoma treatment. Cytotherapy, 18, 828–837.
Sous Naasani, L. I., Rodrigues, C., Azevedo, J. G., Damo Souza, A. F., Buchner, S., & Wink, M. R. (2018). Comparison of human denuded amniotic membrane and porcine small intestine submucosa as scaffolds for Limbal Mesenchymal stem cells. Stem Cell Rev Reports, 14, 744–754.
Rodrigues, C., Naasani, L. I. S., Zanatelli, C., Paim, T. C., Azevedo, J. G., de Lima, J. C., da Cruz Fernandes, M., Buchner, S., & Wink, M. R. (2019). Bioglass 45S5: Structural characterization of short range order and analysis of biocompatibility with adipose-derived mesenchymal stromal cells in vitro and in vivo. Materials Science and Engineering: C, 103, 109781.
Sous Naasani, L. I., Damo Souza, A. F., Rodrigues, C., Vedovatto, S., Azevedo, J. G., Santin Bertoni, A. P., da Cruz Fernandes, M., Buchner, S., & Wink, M. R. (2019). Decellularized human amniotic membrane associated with adipose derived mesenchymal stromal cells as a bioscaffold: Physical, histological and molecular analysis. Biochemical Engineering Journal, 152, 107366.
Glaser, T., Cappellari, A. R., Pillat, M. M., Iser, I. C., Wink, M. R., Battastini, A. M. O., & Ulrich, H. (2012). Perspectives of purinergic signaling in stem cell differentiation and tissue regeneration. Purinergic Signal, 8, 523–537.
Naji, A., Eitoku, M., Favier, B., Deschaseaux, F., Rouas-Freiss, N., & Suganuma, N. (2019). Biological functions of mesenchymal stem cells and clinical implications. Cellular and Molecular Life Sciences, 76, 3323–3348.
Andrzejewska, A., Lukomska, B., & Janowski, M. (2019). Concise review: Mesenchymal stem cells: From roots to boost. Stem Cells, 37, 855–864.
Oedayrajsingh-Varma, M. J., van Ham, S. M., Knippenberg, M., Helder, M. N., Klein-Nulend, J., Schouten, T. E., Ritt, M. J. P. F., & van Milligen, F. J. (2006). Adipose tissue-derived mesenchymal stem cell yield and growth characteristics are affected by the tissue-harvesting procedure. Cytotherapy, 8, 166–177.
Turinetto, V., Vitale, E., & Giachino, C. (2016). Senescence in human mesenchymal stem cells: Functional changes and implications in stem cell-based therapy. International Journal of Molecular Sciences, 17(7), 1164.
Wagner, W., Horn, P., Castoldi, M., Diehlmann, A., Bork, S., Saffrich, R., Benes, V., Blake, J., Pfister, S., Eckstein, V., & Ho, A. D. (2008). Replicative senescence of mesenchymal stem cells: A continuous and organized process. PLoS One, 3(5), e2213.
Baxter, M. A. (2004). Study of telomere length reveals rapid aging of human marrow stromal cells following in vitro expansion. Stem Cells, 22, 675–682.
Lee, W. Y. W., Zhang, T., Lau, C. P. Y., Wang, C. C., Chan, K. M., & Li, G. (2013). Immortalized human fetal bone marrow-derived mesenchymal stromalcell expressing suicide gene for anti-tumor therapy in vitro andin vivo. Cytotherapy, 15, 1484–1497.
Nishioka, K., Fujimori, Y., Hashimoto-Tamaoki, T., Kai, S., Qiu, H., Kobayashi, N., Tanaka, N., Westerman, K. A., Leboulch, P., & Hara, H. (2003). Immortalization of bone marrow-derived human mesenchymal stem cells by removable simian virus 40T antigen gene: Analysis of the ability to support expansion of cord blood hematopoietic progenitor cells. International Journal of Oncology, 23, 925–932.
Hung, S. C., Yang, D. M., Chang, C. F., Lin, R. J., Wang, J. S., Low-Tone Ho, L., & Yang, W. K. (2004). Immortalization without neoplastic transformation of human mesenchymal stem cells by transduction with HPV16 E6/E7 genes. International Journal of Cancer, 110, 313–319.
Balducci, L., Blasi, A., Saldarelli, M., Soleti, A., Pessina, A., Bonomi, A., Coccè, V., Dossena, M., Tosetti, V., Ceserani, V., Navone, S., Falchetti, M., Parati, E., & Alessandri, G. (2014). Immortalization of human adipose-derived stromal cells: Production of cell lines with high growth rate, mesenchymal marker expression and capability to secrete high levels of angiogenic factors. Stem Cell Research & Therapy, 5(3), 63.
Piper, S. L., Wang, M., Yamamoto, A., Malek, F., Luu, A., Kuo, A. C., & Kim, H. T. (2012). Inducible immortality in hTERT-human mesenchymal stem cells. Journal of Orthopaedic Research, 30, 1879–1885.
Bodnar AG, Ouellette M, Frolkis M, et al (1998) Extension of life-span by introduction of telomerase into normal human cells. Science (80- ) 279:349–352.
Lu, S., Wang, J., Ye, J., Zou, Y., Zhu, Y., Wei, Q., Wang, X., Tang, S., Liu, H., Fan, J., Zhang, F., Farina, E. M., Mohammed, M. M., Song, D., Liao, J., Huang, J., Guo, D., Lu, M., Liu, F., Liu, J., Li, L., Ma, C., Hu, X., Lee, M. J., Reid, R. R., Ameer, G. A., Zhou, D., & He, T. (2016). Bone morphogenetic protein 9 (BMP9) induces effective bone formation from reversibly immortalized multipotent adipose-derived (iMAD) mesenchymal stem cells. American Journal of Translational Research, 8, 3710–3730.
Hu, X., Li, L., Yu, X., Zhang, R., Yan, S., Zeng, Z., Shu, Y., Zhao, C., Wu, X., Lei, J., Li, Y., Zhang, W., Yang, C., Wu, K., Wu, Y., An, L., Huang, S., Ji, X., Gong, C., Yuan, C., Zhang, L., Liu, W., Huang, B., Feng, Y., Zhang, B., Haydon, R. C., Luu, H. H., Reid, R. R., Lee, M. J., Wolf, J. M., Yu, Z., & He, T. C. (2017). CRISPR/Cas9-mediated reversibly immortalized mouse bone marrow stromal stem cells (BMSCs) retain multipotent features of mesenchymal stem cells (MSCs). Oncotarget, 8, 111847–111865.
Harley, C. B. (2002). Telomerase is not an oncogene. Oncogene, 21, 494–502.
Jiang, X. R., Jimenez, G., Chang, E., Frolkis, M., Kusler, B., Sage, M., Beeche, M., Bodnar, A. G., Wahl, G. M., Tlsty, T. D., & Chiu, C. P. (1999). Telomerase expression in human somatic cells does not induce changes associated with a transformed phenotype. Nature Genetics, 21, 111–1114.
Kassem, M., Abdallah, B. M., Yu, Z., Ditzel, N., & Burns, J. S. (2004). The use of hTERT-immortalized cells in tissue engineering. Cytotechnology, 45, 39–46.
Huang, G. P., Pan, Z. J., Huang, J. P., Yang, J. F., Guo, C. J., Wang, Y. G., Zheng, Q., Chen, R., Xu, Y. L., Wang, G. Z., Xi, Y. M., Shen, D., Jin, J., & Wang, J. F. (2008). Proteomic analysis of human bone marrow mesenchymal stem cells transduced with human telomerase reverse transcriptase gene during proliferation. Cell Proliferation, 41, 625–644.
Burnstock, G. (2018). The therapeutic potential of purinergic signalling. Biochemical Pharmacology, 151, 157–165.
de Oliveira, B. M., Carvalho, J. L., & Saldanha-Araujo, F. (2016). Adenosine production: A common path for mesenchymal stem-cell and regulatory T-cell-mediated immunosuppression. Purinergic Signal, 12, 595–609.
Kaebisch, C., Schipper, D., Babczyk, P., & Tobiasch, E. (2015). The role of purinergic receptors in stem cell differentiation. Computational and Structural Biotechnology Journal, 13, 75–84.
Roszek, K., & Wujak, M. (2018). How to influence the mesenchymal stem cells fate? Emerging role of ectoenzymes metabolizing nucleotides. Journal of Cellular Physiology, 234, 320–334.
Ferrari Davide D, Gulinelli S, Salvestrini V, et al (2011) Purinergic stimulation of human mesenchymal stem cells potentiates their chemotactic response to CXCL12 and increases the homing capacity and production of proinflammatory cytokines. Exp Hematol 39:360-374.e5.
Coppi E, Pugliese AM, Urbani S, et al (2007) ATP modulates cell proliferation and elicits two different electrophysiological responses in human Mesenchymal stem cells. Stem Cells 25:1840–1849.
Ciciarello, M., Zini, R., Rossi, L., et al. (2012). Extracellular purines promote the differentiation of human bone marrow-derived Mesenchymal stem cells to the Osteogenic and Adipogenic lineages. Stem Cells and Development, 22, 1097–1111.
Counter, C. M., Hahn, W. C., Wei, W., Caddle, S. D., Beijersbergen, R. L., Lansdorp, P. M., Sedivy, J. M., & Weinberg, R. A. (1998). Dissociation among in vitro telomerase activity, telomere maintenance, and cellular immortalization. Proceedings of the National Academy of Sciences of the United States of America, 95, 14723–14728.
Tamajusuku, A. S. K., Villodre, E. S., Paulus, R., Coutinho-Silva, R., Battasstini, A. M. O., Wink, M. R., & Lenz, G. (2010). Characterization of ATP-induced cell death in the GL261 mouse glioma. Journal of Cellular Biochemistry, 109, 983–991.
Albesiano, E., Messmer, B. T., Damle, R. N., et al. (2003). Activation induced cytidine deaminase in chronic lymphocytic leukemia B cells: Expression as multiple forms in a dynamic, variably sized fraction of the clone. Neoplasia, 102, 3333–3340.
Wink, M. R., Braganhol, E., Tamajusuku, A. S. K. K., et al. (2003). Extracellular adenine nucleotides metabolism in astrocyte cultures from different brain regions. Neurochemistry International, 43, 621–628.
Chan, K. M., Delfert, D., & Junger, K. D. (1986). A direct colorimetric assay for Ca2+ −stimulated ATPase activity. Analytical Biochemistry, 157, 375–380.
Bradford, M. M. (1976). A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Analytical Biochemistry, 72, 248–254.
Galanti, B., & Giusti, G. (1966). Direct colorimetric method for the determination of adenosine deaminase and 5-AMP deaminase in the blood. Bollettino della Società Italiana di Biologia Sperimentale, 42, 1316–1320.
Iser IC, Ceschini SM, Onzi GR, et al (2015) Conditioned medium from adipose-derived stem cells ( ADSCs ) promotes epithelial-to-mesenchymal-like transition ( EMT-Like ) in glioma cells in vitro. 53 (10):7184–7199.
Peng, H., Hao, Y., Mousawi, F., Roger, S., Li, J., Sim, J. A., Ponnambalam, S., Yang, X., & Jiang, L. H. (2016). Purinergic and store-operated Ca 2+ signaling mechanisms in Mesenchymal stem cells and their roles in ATP-induced stimulation of cell migration. Stem Cells, 34, 2102–2114.
Jiang, L. H., Mousawi, F., Yang, X., & Roger, S. (2017). ATP-induced Ca2+−signalling mechanisms in the regulation of mesenchymal stem cell migration. Cellular and Molecular Life Sciences, 74, 3697–3710.
Saldanha-Araujo, F., Ferreira, F. I. S., Palma, P. V., Araujo, A. G., Queiroz, R. H. C., Covas, D. T., Zago, M. A., & Panepucci, R. A. (2011). Mesenchymal stromal cells up-regulate CD39 and increase adenosine production to suppress activated T-lymphocytes. Stem Cell Research, 7, 66–74.
Sattler, C., Steinsdoerfer, M., Offers, M., Fischer, E., Schierl, R., Heseler, K., Däubener, W., & Seissler, J. (2011). Inhibition of T-cell proliferation by murine multipotent mesenchymal stromal cells is mediated by CD39 expression and adenosine generation. Cell Transplantation, 20, 1221–1230.
Cavaliere, F., Donno, C., & Ambrosi, N. (2015). Purinergic signaling: A common pathway for neural and mesenchymal stem cell maintenance and differentiation. Frontiers in Cellular Neuroscience, 9, 1–8.
Zippel, N., Limbach, C. A., Ratajski, N., et al. (2011). Purinergic receptors influence the differentiation of human Mesenchymal stem cells. Stem Cells and Development, 21, 884–900.
Bernardo, M. E., Pagliara, D., & Locatelli, F. (2012). Mesenchymal stromal cell therapy: A revolution in regenerative medicine? Bone Marrow Transplantation, 47, 164–171.
Jiang, W., & Xu, J. (2019). Immune modulation by mesenchymal stem cells. Cell Proliferation, 53(1), e12712.
Gao, F., Chiu, S. M., Motan, D. A. L., Zhang, Z., Chen, L., Ji, H. L., Tse, H. F., Fu, Q. L., & Lian, Q. (2016). Mesenchymal stem cells and immunomodulation: Current status and future prospects. Cell Death & Disease, 7(1), e2062.
Nakahara, H., Misawa, H., Hayashi, T., Kondo, E., Yuasa, T., Kubota, Y., Seita, M., Kawamoto, H., Hassan, W. A. R. A., Hassan, R. A. R. A., Javed, S. M., Tanaka, M., Endo, H., Noguchi, H., Matsumoto, S., Takata, K., Tashiro, Y., Nakaji, S., Ozaki, T., & Kobayashi, N. (2009). Bone repair by transplantation of hTERT-immortalized human mesenchymal stem cells in mice. Transplantation, 88, 346–353.
Burns, J. S., Rasmussen, P. L., Larsen, K. H., Schrøder, H. D., & Kassem, M. (2010). Parameters in three-dimensional Osteospheroids of Telomerized human Mesenchymal (stromal) stem cells grown on Osteoconductive scaffolds that predict In Vivo bone-forming potential. Tissue Engineering. Part A, 16, 2331–2342.
Honma, T., Honmou, O., Iihoshi, S., Harada, K., Houkin, K., Hamada, H., & Kocsis, J. D. (2006). Intravenous infusion of immortalized human mesenchymal stem cells protects against injury in a cerebral ischemia model in adult rat. Experimental Neurology, 199, 56–66.
Zhao, F., Qu, Y., Liu, H., du, B., & Mu, D. (2014). Umbilical cord blood mesenchymal stem cells co-modified by TERT and BDNF: A novel neuroprotective therapy for neonatal hypoxic-ischemic brain damage. International Journal of Developmental Neuroscience, 38, 147–154.
Li, J., Liu, W., & Yao, W. (2019). Immortalized human bone marrow derived stromal cells in treatment of transient cerebral ischemia in rats. J Alzheimer’s Dis, 69, 871–880.
Weber, C., Pohl, S., Poertner, R., et al. (2008). Development of a production process for stem cell based cell therapeutic implants using disposable bioreactor systems. In IFMBE proceedings (pp. 2277–2280). Berlin, Heidelberg: Springer.
Siska, E. K., Weisman, I., Romano, J., Ivics, Z., Izsvák, Z., Barkai, U., Petrakis, S., & Koliakos, G. (2017). Generation of an immortalized mesenchymal stem cell line producing a secreted biosensor protein for glucose monitoring. PLoS One, 12(9), e0185498.
Chiu, C.-H., Chang, T.-H., Chang, S.-S., Chang, G. J., Chen, A. C. Y., Cheng, C. Y., Chen, S. C., Fu, J. F., Wen, C. J., & Chan, Y. S. (2020). Application of bone marrow–derived Mesenchymal stem cells for muscle healing after contusion injury in mice. The American Journal of Sports Medicine, 48(5), 1226–1235.
Zhu, G. Q., Jeon, S. H., Lee, K. W., et al. (2020). Engineered stem cells improve neurogenic bladder by overexpressing SDF-1 in a pelvic nerve injury rat model. Cell Transplantation, 29, 963689720902466.
Bourgine, P., Le Magnen, C., Pigeot, S., et al. (2014). Combination of immortalization and inducible death strategies to generate a human mesenchymal stromal cell line with controlled survival. Stem Cell Research, 12, 584–598.
Ge, W., Jiang, J., Arp, J., Liu, W., Garcia, B., & Wang, H. (2010). Regulatory T-cell generation and kidney allograft tolerance induced by mesenchymal stem cells associated with indoleamine 2,3-dioxygenase expression. Transplantation, 90, 1312–1320.
Lotfi, R., Steppe, L., Hang, R., Rojewski, M., Massold, M., Jahrsdörfer, B., & Schrezenmeier, H. (2018). ATP promotes immunosuppressive capacities of mesenchymal stromal cells by enhancing the expression of indoleamine dioxygenase. Immunity, Inflammation and Disease, 6, 448–455.
Toki, Y., Takenouchi, T., Harada, H., Tanuma, S. I., Kitani, H., Kojima, S., & Tsukimoto, M. (2015). Extracellular ATP induces P2X7 receptor activation in mouse Kupffer cells, leading to release of IL-1β, HMGB1, and PGE2, decreased MHC class I expression and necrotic cell death. Biochemical and Biophysical Research Communications, 458, 771–776.
Ulker, P., Özen, N., Abdullayeva, G., Köksoy, S., Yaraş, N., & Basrali, F. (2018). Extracellular ATP activates eNOS and increases intracellular NO generation in red blood cells. Clinical Hemorheology and Microcirculation, 68, 89–101.
Ren, G., Zhang, L., Zhao, X., Xu, G., Zhang, Y., Roberts, A. I., Zhao, R. C., & Shi, Y. (2008). Mesenchymal stem cell-mediated immunosuppression occurs via concerted action of chemokines and nitric oxide. Cell Stem Cell, 2, 141–150.
Jin, L., Zhang, J., Deng, Z., Liu, J., Han, W., Chen, G., Si, Y., & Ye, P. (2020). Mesenchymal stem cells ameliorate myocardial fibrosis in diabetic cardiomyopathy via the secretion of prostaglandin E2. Stem Cell Research & Therapy, 11, 122.
Kerkela; E, Laitinen A, Rabina J, et al (2016) Adenosinergic immunosuppression by human Mesenchymal stromal cells requires co-operation with T cells. Stem Cell 34:781–790.
Sivanathan, K. N., Rojas-Canales, D. M., Hope, C. M., Krishnan, R., Carroll, R. P., Gronthos, S., Grey, S. T., & Coates, P. T. (2015). Interleukin-17A-induced human Mesenchymal stem cells are superior modulators of immunological function. Stem Cells, 33, 2850–2863.
Chatterjee, D., Tufa, D. M., Baehre, H., et al. (2014). Natural killer cells acquire CD73 expression upon exposure to mesenchymal stem cells we. Blood, 123, 595–597.
Lee, J. J., Jeong, H. J., Kim, M. K., Wee, W. R., Lee, W. W., Kim, S. U., Sung, C., & Yang, Y. H. (2014). CD39-mediated effect of human bone marrow-derived mesenchymal stem cells on the human Th17 cell function. Purinergic Signal, 10, 357–365.
Monguió-Tortajada, M., Roura, S., Gálvez-Montón, C., et al. (2017). Mesenchymal stem cells induce expression of CD73 in human monocytes in vitro and in a swine model of myocardial infarction in vivo. Frontiers in Immunology, 8, 1–13.
Amarnath S, Foley JE, Farthing DE, et al (2015) Bone marrow derived Mesenchymal stromal cells harness Purinergenic signaling to Tolerize human Th1 cells in vivo. Stem cell 1200–1212.
Shin, E. Y., Wang, L., Zemskova, M., et al. (2018). Adenosine production by biomaterial-supported mesenchymal stromal cells reduces the innate inflammatory response in myocardial ischemia/reperfusion injury. Journal of the American Heart Association, 7(2), e006949.
Tan, K., Zhu, H., Zhang, J., et al. (2019). CD73 expression on mesenchymal stem cells dictates the reparative properties via its anti-inflammatory activity. Stem Cells International, 2019, 8717694.
Rodriguez, R., Rosu-Myles, M., Aráuzo-Bravo, M., Horrillo, A., Pan, Q., Gonzalez-Rey, E., Delgado, M., & Menendez, P. (2014). Human bone marrow stromal cells lose immunosuppressive and anti-inflammatory properties upon oncogenic transformation. Stem Cell Reports, 3, 606–619.
Antonioli L, Blandizzi C, Pacher P, Haskó G (2013) Immunity , inflammation and cancer : a leading role for adenosine. Nat Publ Gr 13:842–857.
Borea, P. A., Gessi, S., Merighi, S., & Varani, K. (2016). Adenosine as a multi-Signalling Guardian angel in human diseases: When, where and how does it exert its protective effects? Trends in Pharmacological Sciences, 37, 419–434.
Dominici, M., Le Blanc, K., Mueller, I., et al. (2006). Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy, 8, 315–317.
Iser IC, Bracco P a., Gonçalves CEI, et al (2014) Mesenchymal stem cells from different murine tissues have differential capacity to metabolize extracellular nucleotides. Journal of Cellular Biochemistry 115:1673–1682.
Naasani, L. I. S., Rodrigues, C., de Campos, R. P., Beckenkamp, L. R., Iser, I. C., Bertoni, A. P. S., & Wink, M. R. (2017). Extracellular nucleotide hydrolysis in dermal and Limbal Mesenchymal stem cells: A source of adenosine production. Journal of Cellular Biochemistry, 118, 2430–2442.
Roszek, K., Bomastek, K., Drożdżal, M., & Komoszyński, M. (2013). Dramatic differences in activity of purines metabolizing ecto-enzymes between mesenchymal stem cells isolated from human umbilical cord blood and umbilical cord tissue. Biochemistry and Cell Biology, 91, 519–525.
Chen, X., Shao, H., Zhi, Y., Xiao, Q., Su, C., Dong, L., Liu, X., Li, X., & Zhang, X. (2016). CD73 pathway contributes to the immunosuppressive ability of Mesenchymal stem cells in intraocular autoimmune responses. Stem Cells and Development, 25, 337–346.
Netsch, P., Elvers-Hornung, S., Uhlig, S., Klüter, H., Huck, V., Kirschhöfer, F., Brenner-Weiß, G., Janetzko, K., Solz, H., Wuchter, P., Bugert, P., & Bieback, K. (2018). Human mesenchymal stromal cells inhibit platelet activation and aggregation involving CD73-converted adenosine. Stem Cell Research & Therapy, 9(1), 184.
Boison, D., & Yegutkin, G. G. (2019). Adenosine metabolism: Emerging concepts for Cancer therapy. Cancer Cell, 36, 582–596.
Rodríguez-Serrano, F., Álvarez, P., Caba, O., et al. (2010). Promotion of human adipose-derived stem cell proliferation mediated by exogenous nucleosides. Cell Biology International, 34, 917–924.
Cader MZ, de Almeida Rodrigues RP, West JA, et al (2020) FAMIN is a multifunctional purine enzyme enabling the purine nucleotide cycle. Cell 180:278-295.e23.
Mousawi, F., Peng, H., Li, J., Ponnambalam, S., Roger, S., Zhao, H., Yang, X., & Jiang, L. H. (2020). Chemical activation of the Piezo1 channel drives mesenchymal stem cell migration via inducing ATP release and activation of P2 receptor purinergic signaling. Stem Cells, 38, 410–421.
Zhou, Q., Yang, C., & Yang, P. (2017). The promotional effect of Mesenchymal stem cell homing on bone tissue regeneration. Current Stem Cell Research & Therapy, 12, 365–376.
Acknowledgements
This study was financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior – Brasil (CAPES) – Finance Code 001; All students are recipients of fellowships from CAPES. MRW, GL and RPC are recipients of research fellowship from Conselho Nacional de Desenvolvimento Científico e Tecnológico - Brasil (CNPq). This study was supported by Fundação de Amparo à Pesquisa do Estado do Rio Grande do Sul - Brasil (FAPERGS/CAPES 06/2018 - Programa de Internacionalização da pós-graduação no RS (19/2551-0000679-9) and FAPERGS/MS/CNPq/SESRS n.03/2017 – PPSUS (17/2551-0001)); and CNPqMS-SCTIE-Decit/CNPqn°12/2018(441575/2018-8). JS received support from the Natural Sciences and Engineering Research Council of Canada (NSERC; RGPIN-2016-05867).
Author information
Authors and Affiliations
Contributions
LRB performed cell culture experiments, HPLC assays, flow cytometry, immunosuppression assay and wrote the manuscript. GRO assisted the stable transfection cell assays and wrote the manuscript. DMF and VGK performed cell culture experiments, enzymatic activity and cell differentiation assay, flow cytometry and doubling population experiments. RPC performed the stable transfection of cells. ICI performed the ADA enzymatic assay. APSB performed RT-qPCR and HPLC assays. JS contributed to the interpretation of the results and provided the NTPDases antibodies. MRW and GL supervised the experiments, assisted in drafting and critical reading. All the authors discussed the results and contributed to the writing of the manuscript.
Corresponding author
Ethics declarations
Disclosure Statement
The authors have no conflict of interest to declare.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 19 kb)
Supplementary Figure 1
– CD73 activity and expression in a new cell transduction with TERT. To confirm that cell immortalization process alters the activity and expression of CD73 enzyme, a new stable transfection with the TERT gene was performed. (A) The TERT gene insertion was confirmed by RT-qPCR, as demonstrated by melt curve peak chart collected using the StepOnePlusTM (Applied Biosystems). (B) Flow cytometry data analysis also confirmed a decrease of CD73 MFI in MSCs-TERT (n = 3). (C) Specific enzymatic activity from MSCs and MSCs-TERT measured by release of inorganic phosphate after incubation with AMP (n = 3). Data are expressed as nmol Pi/min/mL, using mean ± SD. T-test was used to determine the statistical difference. (PNG 285 kb)
Rights and permissions
About this article
Cite this article
Beckenkamp, L.R., da Fontoura, D.M.S., Korb, V.G. et al. Immortalization of Mesenchymal Stromal Cells by TERT Affects Adenosine Metabolism and Impairs their Immunosuppressive Capacity. Stem Cell Rev and Rep 16, 776–791 (2020). https://doi.org/10.1007/s12015-020-09986-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-020-09986-5