Abstract
Background
Long-term outcomes of endoscopic submucosal dissection (ESD) for esophageal squamous cell carcinoma (ESCC) have not been assessed in a large, multicenter cohort. We aimed to evaluate long-term outcomes of ESD for ESCC in a real-world setting.
Methods
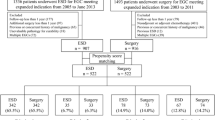
We retrospectively recruited 659 patients who underwent ESD for ESCC at ten institutions from January 2007 to December 2015. Of these, 566 patients were analyzed and classified into three groups according to the pathologic invasion depth after ESD: epithelium/lamina propria mucosa (EP/LPM group: 454 patients), muscularis mucosa/submucosa invasion ≤ 200 μm below the inferior margin of the muscularis mucosa (MM/SM1 group: 81 patients), and submucosa invasion > 200 μm below the MM inferior margin (SM2 group: 31 patients).
Results
The 5-year overall survival rates in the EP/LPM, MM/SM1, and SM2 groups were 92.6%, 80.0%, and 62.7%, respectively, while the 5-year disease-specific survival rates were 99.7%, 96.9%, and 88.3%, respectively. Multivariate analyses revealed that the invasion depth, Charlson Comorbidity Index (CCI), and prognostic nutritional index (PNI) were independent prognostic factors. Hazard ratios in the MM/SM1 and SM2 groups were 2.25 (95% confidence interval [CI] 1.04–4.83; P = 0.038) and 3.18 (95% CI 1.08–9.34; P = 0.036), respectively, compared to those in the EP/LPM group, while those for patients with a CCI ≥ 3 and PNI ≤ 47.75 were 3.25 (95% CI 1.79–5.89; P < 0.001) and 2.42 (95% CI 1.26–4.65; P = 0.008), respectively.
Conclusions
This study identified that invasion depth, presence of comorbid diseases and preoperative nutritional status are independent prognostic risk factors associated with ESCC patients undergoing ESD.




Similar content being viewed by others
References
Arnold M, Soerjomataram I, Ferlay J, Forman D (2015) Global incidence of oesophageal cancer by histological subtype in 2012. Gut 64:381–387
Abnet CC, Arnold M, Wei WQ (2018) Epidemiology of esophageal squamous cell carcinoma. Gastroenterology 154:360–373
Gupta B, Kumar N (2017) Worldwide incidence, mortality and time trends for cancer of the oesophagus. Eur J Cancer Prev 26:107–118
Tachimori Y, Ozawa S, Numasaki H, Ishihara R, Matsubara H, Muro K, Oyama T, Toh Y, Udagawa H, Uno T (2018) Comprehensive registry of esophageal cancer in Japan, 2011. Esophagus 15:127–152
Oyama T, Tomori A, Hotta K, Morita S, Kominato K, Tanaka M, Miyata Y (2005) Endoscopic submucosal dissection of early esophageal cancer. Clin Gastroenterol Hepatol 3:S67-70
Fujishiro M, Yahagi N, Kakushima N, Kodashima S, Muraki Y, Ono S, Yamamichi N, Tateishi A, Shimizu Y, Oka M, Ogura K, Kawabe T, Ichinose M, Omata M (2006) Endoscopic submucosal dissection of esophageal squamous cell neoplasms. Clin Gastroenterol Hepatol 4:688–694
Ishihara R, Iishi H, Uedo N, Takeuchi Y, Yamamoto S, Yamada T, Masuda E, Higashino K, Kato M, Narahara H, Tatsuta M (2008) Comparison of EMR and endoscopic submucosal dissection for en bloc resection of early esophageal cancers in Japan. Gastrointest Endosc 68:1066–1072
Takahashi H, Arimura Y, Masao H, Okahara S, Tanuma T, Kodaira J, Kagaya H, Shimizu Y, Hokari K, Tsukagoshi H, Shinomura Y, Fujita M (2010) Endoscopic submucosal dissection is superior to conventional endoscopic resection as a curative treatment for early squamous cell carcinoma of the esophagus (with video). Gastrointest Endosc 72(255–264):264.e251–252
Yamashina T, Ishihara R, Nagai K, Matsuura N, Matsui F, Ito T, Fujii M, Yamamoto S, Hanaoka N, Takeuchi Y, Higashino K, Uedo N, Iishi H (2013) Long-term outcome and metastatic risk after endoscopic resection of superficial esophageal squamous cell carcinoma. Am J Gastroenterol 108:544–551
Nakagawa K, Koike T, Iijima K, Shinkai H, Hatta W, Endo H, Ara N, Uno K, Asano N, Imatani A, Shimosegawa T (2014) Comparison of the long-term outcomes of endoscopic resection for superficial squamous cell carcinoma and adenocarcinoma of the esophagus in Japan. Am J Gastroenterol 109:348–356
Berger A, Rahmi G, Perrod G, Pioche M, Canard JM, Cesbron-Metivier E, Boursier J, Samaha E, Vienne A, Lepilliez V, Cellier C (2019) Long-term follow-up after endoscopic resection for superficial esophageal squamous cell carcinoma: a multicenter Western study. Endoscopy 51:298–306
Ono S, Fujishiro M, Niimi K, Goto O, Kodashima S, Yamamichi N, Omata M (2009) Long-term outcomes of endoscopic submucosal dissection for superficial esophageal squamous cell neoplasms. Gastrointest Endosc 70:860–866
Repici A, Hassan C, Carlino A, Pagano N, Zullo A, Rando G, Strangio G, Romeo F, Nicita R, Rosati R, Malesci A (2010) Endoscopic submucosal dissection in patients with early esophageal squamous cell carcinoma: results from a prospective Western series. Gastrointest Endosc 71:715–721
Joo DC, Kim GH, Park DY, Jhi JH, Song GA (2014) Long-term outcome after endoscopic submucosal dissection in patients with superficial esophageal squamous cell carcinoma: a single-center study. Gut and liver 8:612–618
Tsujii Y, Nishida T, Nishiyama O, Yamamoto K, Kawai N, Yamaguchi S, Yamada T, Yoshio T, Kitamura S, Nakamura T, Nishihara A, Ogiyama H, Nakahara M, Komori M, Kato M, Hayashi Y, Shinzaki S, Iijima H, Michida T, Tsujii M, Takehara T (2015) Clinical outcomes of endoscopic submucosal dissection for superficial esophageal neoplasms: a multicenter retrospective cohort study. Endoscopy 47:775–783
Nagami Y, Ominami M, Shiba M, Minamino H, Fukunaga S, Kameda N, Sugimori S, Machida H, Tanigawa T, Yamagami H, Watanabe T, Tominaga K, Fujiwara Y, Arakawa T (2017) The five-year survival rate after endoscopic submucosal dissection for superficial esophageal squamous cell neoplasia. Dig Liver Dis 49:427–433
Ohashi S, Miyamoto S, Kikuchi O, Goto T, Amanuma Y, Muto M (2015) Recent advances from basic and clinical studies of esophageal squamous cell carcinoma. Gastroenterology 149:1700–1715
Kitagawa Y, Uno T, Oyama T, Kato K, Kato H, Kawakubo H, Kawamura O, Kusano M, Kuwano H, Takeuchi H, Toh Y, Doki Y, Naomoto Y, Nemoto K, Booka E, Matsubara H, Miyazaki T, Muto M, Yanagisawa A, Yoshida M (2019) Esophageal cancer practice guidelines 2017 edited by the Japan Esophageal Society: part 1. Esophagus 16:1–24
Secretan B, Straif K, Baan R, Grosse Y, El Ghissassi F, Bouvard V, Benbrahim-Tallaa L, Guha N, Freeman C, Galichet L, Cogliano V (2009) A review of human carcinogens—Part E: tobacco, areca nut, alcohol, coal smoke, and salted fish. Lancet Oncol 10:1033–1034
Ishihara R, Tanaka H, Iishi H, Takeuchi Y, Higashino K, Uedo N, Tatsuta M, Yano M, Ishiguro S (2008) Long-term outcome of esophageal mucosal squamous cell carcinoma without lymphovascular involvement after endoscopic resection. Cancer 112:2166–2172
Sato Y, Motoyama S, Maruyama K, Okuyama M, Ogawa J (2005) A second malignancy is the major cause of death among thoracic squamous cell esophageal cancer patients negative for lymph node involvement. J Am Coll Surg 201:188–193
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Onodera T, Goseki N, Kosaki G (1984) Prognostic nutritional index in gastrointestinal surgery of malnourished cancer patients. Nihon Geka Gakkai zasshi 85:1001–1005
Forrest LM, McMillan DC, McArdle CS, Angerson WJ, Dunlop DJ (2003) Evaluation of cumulative prognostic scores based on the systemic inflammatory response in patients with inoperable non-small-cell lung cancer. Br J Cancer 89:1028–1030
Toiyama Y, Miki C, Inoue Y, Tanaka K, Mohri Y, Kusunoki M (2011) Evaluation of an inflammation-based prognostic score for the identification of patients requiring postoperative adjuvant chemotherapy for stage II colorectal cancer. Exp Ther Med 2:95–101
Fairclough E, Cairns E, Hamilton J, Kelly C (2009) Evaluation of a modified early warning system for acute medical admissions and comparison with C-reactive protein/albumin ratio as a predictor of patient outcome. Clin Med (Lond) 9:30–33
Halazun KJ, Hardy MA, Rana AA, Woodland DC, Luyten EJ, Mahadev S, Witkowski P, Siegel AB, Brown Jr. RS, Emond JC, (2009) Negative impact of neutrophil-lymphocyte ratio on outcome after liver transplantation for hepatocellular carcinoma. Ann Surg 250:141–151
Nakajo K, Abe S, Oda I, Ishihara R, Tanaka M, Yoshio T, Katada C, Yano T (2019) Impact of the Charlson Comorbidity Index on the treatment strategy and survival in elderly patients after non-curative endoscopic submucosal dissection for esophageal squamous cell carcinoma: a multicenter retrospective study. J Gastroenterol 54:871–880
Takahashi K, Hashimoto S, Mizuno KI, Kobayashi T, Tominaga K, Sato H, Kohisa J, Ikarashi S, Hayashi K, Takeuchi M, Yokoyama J, Kawai H, Sato Y, Kobayashi M, Terai S (2018) Management decision based on lymphovascular involvement leads to favorable outcomes after endoscopic treatment of esophageal squamous cell carcinoma. Endoscopy 50:662–670
Kudou M, Shiozaki A, Fujiwara H, Konishi H, Shoda K, Arita T, Kosuga T, Morimura R, Murayama Y, Kuriu Y, Ikoma H, Kubota T, Nakanishi M, Okamoto K, Dohi O, Konishi H, Naito Y, Otsuji E (2017) Efficacy of additional surgical resection after endoscopic submucosal dissection for superficial esophageal cancer. Anticancer Res 37:5301–5307
Suzuki G, Yamazaki H, Aibe N, Masui K, Sasaki N, Shimizu D, Kimoto T, Shiozaki A, Dohi O, Fujiwara H, Ishikawa T, Konishi H, Naito Y, Otsuji E, Yamada K (2018) Endoscopic submucosal dissection followed by chemoradiotherapy for superficial esophageal cancer: choice of new approach. Radiat Oncol 13:246
Slaughter DP, Southwick HW, Smejkal W (1953) Field cancerization in oral stratified squamous epithelium; clinical implications of multicentric origin. Cancer 6:963–968
Minashi K, Nihei K, Mizusawa J, Takizawa K, Yano T, Ezoe Y, Tsuchida T, Ono H, Iizuka T, Hanaoka N, Oda I, Morita Y, Tajika M, Fujiwara J, Yamamoto Y, Katada C, Hori S, Doyama H, Oyama T, Nebiki H, Amagai K, Kubota Y, Nishimura K, Kobayashi N, Suzuki T, Hirasawa K, Takeuchi T, Fukuda H, Muto M (2019) Efficacy of endoscopic resection and selective chemoradiotherapy for stage I esophageal squamous cell carcinoma. Gastroenterology 157(2):382–390
Vashist YK, Loos J, Dedow J, Tachezy M, Uzunoglu G, Kutup A, Yekebas EF, Izbicki JR (2011) Glasgow Prognostic Score is a predictor of perioperative and long-term outcome in patients with only surgically treated esophageal cancer. Ann Surg Oncol 18:1130–1138
Xu XL, Yu HQ, Hu W, Song Q, Mao WM (2015) A novel inflammation-based prognostic score, the C-reactive protein/albumin ratio predicts the prognosis of patients with operable esophageal squamous cell carcinoma. PLoS ONE 10:e0138657
Sharaiha RZ, Halazun KJ, Mirza F, Port JL, Lee PC, Neugut AI, Altorki NK, Abrams JA (2011) Elevated preoperative neutrophil: lymphocyte ratio as a predictor of postoperative disease recurrence in esophageal cancer. Ann Surg Oncol 18:3362–3369
Acknowledgements
We thank all members of the KESG. We are also grateful to the following investigators: Tsugitaka Ishida, Yuka Azuma, Hiroaki Kitae, Shinya Matsumura, Kazuyuki Ogita, Shun Takayama, Naoki Mizuno (Kyoto Prefectural University of Medicine), and Takahiro Nakano (Japanese Red Cross Society Kyoto Daiichi Hospital) for their help with the data collection.
Funding
This work was partly supported by Grants-in-Aid for JFE (The Japanese Foundation for Research and Promotion of Endoscopy) Grant to Osamu Dohi and Cancer Research Grant from Kyoto Preventive Medical Center to Naoto Iwai.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Naoto Iwai, Osamu Dohi, Shinya Yamada, Akihito Harusato, Ryusuke Horie, Takeshi Yasuda, Nobuhisa Yamada, Yusuke Horii, Atsushi Majima, Keika Zen, Hiroyuki Kimura, Nobuaki Yagi, Yuji Naito, and Yoshito Itoh have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Iwai, N., Dohi, O., Yamada, S. et al. Prognostic risk factors associated with esophageal squamous cell carcinoma patients undergoing endoscopic submucosal dissection: a multi-center cohort study. Surg Endosc 36, 2279–2289 (2022). https://doi.org/10.1007/s00464-021-08502-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08502-1