Abstract
Purpose
The sensitivity of Gram staining is known to be suboptimal for the diagnosis of native joint septic arthritis. We lack information about the accuracy of Gram compared to other microscopic staining techniques for predicting infection in different patient populations.
Methods
This was a cohort study with cost evaluations at the Orthopaedic Service of Geneva University Hospitals (January 1996–October 2012).
Results
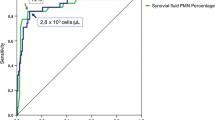
Among 500 episodes of arthritis (196 with immunosuppression, 227 with underlying arthroplasties and 69 with gout or other crystals in synovial fluid), Gram staining revealed pathogens in 146 episodes (146/500, 29 %) or in 146 of the 400 culture-positive episodes (37 %). Correlation between the Gram and acridine staining of the same sample was good (Spearman 0.85). Overall, the sensitivity, specificity, positive predictive value and negative predictive value of Gram stain for rapid diagnosis of septic arthritis was 0.37, 0.99, 0.99 and 0.28, respectively, compared to microbiological cultures. Quite similar values were recorded across the different patient subpopulations, in particular for sensitivity values that were 0.33 for patients with prosthetic joint infections, 0.40 for immunosuppressed patients, 0.36 for patients under antibiotic administration and 0.52 for patients with concomitant crystalline disease.
Conclusions
The sensitivity of Gram or acridine orange staining for a rapid diagnosis of episodes of septic arthritis is suboptimal compared to microbiological culture, regardless of underlying conditions, immunosuppression or antibiotic therapy. The sensitivity in the presence of synovial fluid crystals is moderate. Acridine orange and Gram stains are equivalent.



Similar content being viewed by others
References
Margaretten ME, Kohlwes J, Moore D, Bent S (2007) Does this adult patient have septic arthritis? JAMA 297:1478–1488
Siva C, Velazquez C, Mody A, Brasington R (2003) Diagnosing acute monoarthritis in adults: a practical approach for the family physician. Am Fam Physician 68:83–90
Brannan SR, Jerrard DA (2006) Synovial fluid analysis. J Emerg Med 30:331–339
Frischnecht J, Steigerwald JC (1975) High synovial fluid white blood cell counts in pseudogout; possible confusion with septic arthritis. Arch Intern Med 135:298–299
Faraj AA, Omonbude OD, Godwin P (2002) Gram staining in the diagnosis of acute septic arthritis. Acta Orthop Belg 68:388–391
McGillicuddy DC, Shah KH, Friedberg RP, Nathanson LA, Edlow JA (2007) How sensitive is the synovial fluid white blood cell count in diagnosing septic arthritis? Am J Emerg Med 25:749–752
Carpenter CR, Schuur JD, Everett WW, Pines JM (2011) Evidence-based diagnostics: adult septic arthritis. Acad Emerg Med 18:781–796
Yu KH, Luo SF, Liou LB, Wu YJ, Tsai WP, Chen JY et al (2003) Concomitant septic and gouty arthritis—an analysis of 30 cases. Rheumatology (Oxford) 42:1062–1066
Brook I, Reza MJ, Bricknell KS, Bluestone R, Finegold SM (1978) Synovial fluid lactic acid. A diagnostic aid in septic arthritis. Arthritis Rheum 21:774–779
Martinot M, Sordet C, Soubrier M, Puéchal X, Saraux A, Lioté F et al (2005) Diagnostic value of serum and synovial procalcitonin in acute arthritis: a prospective study of 42 patients. Clin Exp Rheumatol 23:303–310
Gardner GC, Weisman MH (1990) Pyarthrosis in patients with rheumatoid arthritis: a report of 13 cases and a review of the literature from the past 40 years. Am J Med 88:503–511
Weng CT, Liu MF, Lin LH, Weng MY, Lee NY, Wu AB et al (2009) Rare coexistence of gouty and septic arthritis: a report of 14 cases. Clin Exp Rheumatol 27:902–906
Hügle T, Schuetz P, Mueller B, Laifer G, Tyndall A, Regenass S et al (2008) Serum procalcitonin for discrimination between septic and non-septic arthritis. Clin Exp Rheumatol 26:453–456
Ernst AA, Weiss SJ, Tracy LA, Weiss NR (2010) Usefulness of CRP and ESR in predicting septic joints. South Med J 103:522–526
Madison BM (2001) Application of stains in clinical microbiology. Biotech Histochem 76:119–125
Hariharan P, Kabrhel C (2011) Sensitivity of erythrocyte sedimentation rate and C-reactive protein for the exclusion of septic arthritis in emergency department patients. J Emerg Med 40:428–431
Morgan PM, Sharkey P, Ghanem E, Parvizi J, Clohisy JC, Burnett RS et al (2009) The value of intraoperative Gram stain in revision total knee arthroplasty. J Bone Joint Surg Am 91:2124–2129
Ciancio G, Bortoluzzi A, Govoni M (2012) Epidemiology of gout and chondrocalcinosis. Reumatismo 63:207–220
Rosenthal AK (2011) Crystals, inflammation, and osteoarthritis. Curr Opin Rheumatol 23:170–173
Papanicolas LE, Hakendorf P, Gordon DL (2012) Concomitant septic arthritis in crystal monoarthritis. J Rheumatol 39:157–160
Archibeck MJ, Rosenberg AG, Sheinkop MB, Berger RA, Jacobs JJ (2001) Gout-induced arthropathy after total knee arthroplasty: a report of two cases. Clin Orthop Relat Res 392:377–382
Performance standards for antimicrobial susceptibility testing: 17th informational supplement M100–S17 (2007) Clinical and Laboratory Standards Institute, Wayne
Vittinghoff E, McCulloch CE (2007) Relaxing the rule of ten events per variable in logistic and Cox regression. Am J Epidemiol 165:710–718
Uçkay I, Harbarth S, Peter R, Lew D, Hoffmeyer P, Pittet D (2010) Preventing surgical site infections. Expert Rev Anti Infect Ther 8:657–670
Bouvet C, Tchernin D, Seirafi M, Stern R, Lew D, Hoffmeyer P et al (2011) No need to search for the source of haematogenous arthroplasty infections. Swiss Med Wkly 141:w13306–w13311
Uçkay I, Bouchuiguir-Wafa K, Ninet B, Emonet S, Assal M, Harbarth S et al (2010) Posttraumatic ankle arthritis due to a novel Nocardia species. Infection 38:407–412
Uçkay I, Garzoni C, Ferry T, Harbarth S, Stern R, Assal M et al (2010) Postoperative serum pro-calcitonin and C-reactive protein levels in patients with orthopedic infections. Swiss Med Wkly 140:w13124–w13129
Acknowledgments
We thank the Orthopaedic Service and the various laboratories for their support.
Conflict of interest
There are no financial supports or other benefits from commercial sources for the work reported on in the manuscript, or any other financial interests that any of the authors may have, which could create a potential conflict of interest or the appearance of a conflict of interest with regard to the work. Parts of the manuscript have been presented as posters and short presentations at the Swiss National Congresses for Infectiology (Lugano, June 2013) and Orthopaedic Surgery (Lausanne, June 2013).
Author information
Authors and Affiliations
Corresponding author
Additional information
Gregory Cunningham and Khalid Seghrouchni contributed equally as first authors.
Rights and permissions
About this article
Cite this article
Cunningham, G., Seghrouchni, K., Ruffieux, E. et al. Gram and acridine orange staining for diagnosis of septic arthritis in different patient populations. International Orthopaedics (SICOT) 38, 1283–1290 (2014). https://doi.org/10.1007/s00264-014-2284-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-014-2284-3