Abstract
Background and purpose
In cases of simultaneous chemoradiotherapy (CRT), early recognition of toxic side effects is important, as drug discontinuation may prevent further injury. It appears favorable to undertake further steps to investigate whether patient subgroups behave differently depending on their toxicity profile.
Methods
We retrospectively analyzed 125 consecutive patients with non-metastasized carcinoma of the head and neck who were treated with CRT (cisplatin 40 mg/m2 weekly) in 2013/2014. Patients were planned to receive six cycles of cisplatin. Statistical analyses were performed using the chi2 test, t-test, Kaplan–Meier method, and the log-rank test, as appropriate.
Results
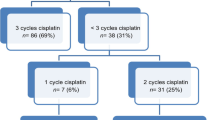
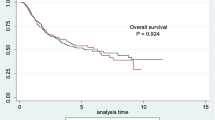
Eighty-six patients did not reach the intended sixth cycle (68.8%; 60.0% of whom were ≥60 years, p < 0.05). Acute kidney injury (glomerular filtration rate <60 mL/min/1.73m2) was the most common reason for drug discontinuation (26.7%; 82.6% of whom were ≥60 years; p < 0.01), followed by leukopenia <3/nL (23.3%; 75% of whom were <60 years; p < 0.01) and infection (11.6%). Patients who underwent ≥5 cycles were associated with prolonged overall survival and metastasis-free survival after CRT (p < 0.02; median follow-up 24 months), especially patients <60 years.
Conclusion
Acute kidney injury was the most common side effect in patients ≥60 years, whereas leukopenia characteristically occurred significantly more often in younger patients. Discontinuing cisplatin during CRT was associated with a worse outcome, especially in patients <60 years.
Zusammenfassung
Hintergrund und Zielsetzung
Bei einer simultanen Radiochemotherapie (CRT) ist eine Früherkennung von toxischen Nebenwirkungen bedeutsam, um weiteren Organschäden vorzubeugen. Hierzu ist wichtig, zu eruieren, ob bestimmte Subgruppen von Patienten ein unterschiedliches Profil ihrer Toxizitäten aufweisen.
Methoden
Es erfolgte eine retrospektive Analyse von 125 konsekutiven Patienten mit nichtfernmetastasierten Kopf-Hals-Tumoren, welche eine CRT (Cisplatin 40 mg/m2 wöchentlich) im Jahr 2013/2014 erhalten hatten. Vorgesehen waren insgesamt 6 Zyklen Cisplatin. Zur statistischen Analyse wurden Chi2-Test, t-Test, Kaplan-Meier-Methode und Log-rank-Test verwendet.
Ergebnisse
Sechsundachtzig Patienten erreichten den geplanten 6. Zyklus nicht (68,8 %; 60,0 % davon ≥60 Jahre; p < 0,05). Ein akutes Nierenversagen (glomeruläre Filtrationsrate <60 ml/min/1,73m2) war der häufigste Grund für eine Unterbrechung der Cisplatin-Gaben (26,7 %; 82,6 % davon ≥60 Jahre; p < 0,01), gefolgt von Leukopenie <3/nl (23,3 %; 75 % davon <60 Jahre; p < 0,01) und Infekt (11,6 %). Patienten, welche ≥5 Zyklen erhielten, wiesen ein verlängertes Gesamt- und metastasenfreies Überleben nach CRT auf (p < 0,02; medianes Follow-up 24 Monate), besonders Patienten <60 Jahre.
Schlussfolgerung
Ein akutes Nierenversagen war die häufigste Nebenwirkung bei Patienten ≥60 Jahre, wohingegen eine Leukopenie charakteristischerweise häufiger bei jüngeren Patienten auftrat. Eine Unterbrechung der Cisplatin-Therapie war mit einem schlechteren Outcome vergesellschaftet, besonders bei Patienten <60 Jahren.




Similar content being viewed by others
References
Bonner JA, Harari PM, Giralt J et al (2006) Radiotherapy plus cetuximab for squamous-cell carcinoma of the head and neck. N Engl J Med 354:567–578
Xiang M, Holsinger FC, Colevas AD, Chen MM, Le QT, Beadle BM (2018) Survival of patients with head and neck cancer treated with definitive radiotherapy and concurrent cisplatin or concurrent cetuximab: a surveillance, epidemiology, and end results-medicare analysis. Cancer 124:4486–4494
Sun XS, Sire C, Tao Y et al (2018) A phase II randomized trial of pembrolizumab versus cetuximab, concomitant with radiotherapy (RT) in locally advanced (LA) squamous cell carcinoma of the head and neck (SCCHN): first results of the GORTEC 2015-01 “PembroRad” trial. J Clin Oncol 36:6018–6018
Gooi Z, Fakhry C, Goldenberg D et al (2016) AHNS Series: Do you know your guidelines?Principles of radiation therapy for head and neck cancer: a review of the National Comprehensive Cancer Network guidelines. Head Neck 38:987–992
Onbasi Y, Lettmaier S, Hecht M et al (2019) Is there a patient population with squamous cell carcinoma of the head and neck region who might benefit from de-intensification of postoperative radiotherapy? Strahlenther Onkol 195:482–495
Tribius S, Meyer MS, Pflug C et al (2018) Socioeconomic status and quality of life in patients with locally advanced head and neck cancer. Strahlenther Onkol 194:737–749
Nieder C, Kampe TA, Pawinski A, Dalhaug A (2018) Patient-reported symptoms before palliative radiotherapy predict survival differences. Strahlenther Onkol 194:533–538
Alterio D, Gerardi MA, Cella L et al (2017) Radiation-induced acute dysphagia: prospective observational study on 42 head and neck cancer patients. Strahlenther Onkol 193:971–981
Korner P, Ehrmann K, Hartmannsgruber J et al (2017) Patient-reported symptoms during radiotherapy: clinically relevant symptom burden in patients treated with palliative and curative intent. Strahlenther Onkol 193:570–577
Grégoire V, Eisbruch A, Hamoir M, Levendag P (2006) Proposal for the delineation of the nodal CTV in the node-positive and the post-operative neck. Radiother Oncol 79:15–20
Grégoire V, Levendag P, Ang KK et al (2003) CT-based delineation of lymph node levels and related CTVs in the node-negative neck: DAHANCA, EORTC, GORTEC, NCIC, RTOG consensus guidelines. Radiother Oncol 69:227–236
Kirkpatrick JP, van der Kogel AJ, Schultheiss TE (2010) Radiation dose—volume effects in the spinal cord. Int J Radiat Oncol Biol Phys 76:S42–S9
Mayo C, Martel MK, Marks LB, Flickinger J, Nam J, Kirkpatrick J (2010) Radiation dose—volume effects of optic nerves and chiasm. Int J Radiat Oncol Biol Phys 76:S28–S35
Deasy JO, Moiseenko V, Marks L, Chao KC, Nam J, Eisbruch A (2010) Radiotherapy dose—volume effects on salivary gland function. Int J Radiat Oncol Biol Phys 76:S58–S63
United Nations (2013) World population ageing 2013. United Nations Publ, New York, USA
Orimo H, Ito H, Suzuki T, Araki A, Hosoi T, Sawabe M (2006) Reviewing the definition of “elderly”. Geriatr Gerontol Int 6:149–158
Peng L, Xu C, Chen Y‑P et al (2019) Optimizing the cumulative cisplatin dose during radiotherapy in nasopharyngeal carcinoma: dose-effect analysis for a large cohort. Oral Oncol 89:102–106
Otty Z, Skinner MB, Dass J et al (2011) Efficacy and tolerability of weekly low-dose cisplatin concurrent with radiotherapy in head and neck cancer patients. Asia-Pac J Clin Oncol 7:287–292
Spreafico A, Huang SH, Xu W et al (2015) Differential impact of cisplatin dose intensity on human papillomavirus (HPV)-related (+) and HPV-unrelated (−) locoregionally advanced head and neck squamous cell carcinoma (LAHNSCC). J Clin Oncol 33:6020–6020
Motwani SS, McMahon GM, Humphreys BD, Partridge AH, Waikar SS, Curhan GC (2018) Development and validation of a risk prediction model for acute kidney injury after the first course of cisplatin. J Clin Oncol 36:682–688
Pignon J‑P, Le Maitre A, Maillard E, Bourhis J, Group M‑NC (2009) Meta-analysis of chemotherapy in head and neck cancer (MACH-NC): an update on 93 randomised trials and 17,346 patients. Radiother Oncol 92:4–14
Melotek JM, Cooper BT, Koshy M, Silverman JS, Spiotto MT (2016) Weekly versus every-three-weeks platinum-based chemoradiation regimens for head and neck cancer. Head Neck Surg 45:62
Becker-Schiebe M, Christiansen H (2018) Wöchentliche oder dreiwöchentliche Cisplatin-Gaben bei der kombinierten Radiochemotherapie lokal fortgeschrittener Kopf-Hals-Tumoren? Strahlenther Onkol 194:468–470
Morse RT, Ganju RG, TenNapel MJ et al (2019) Weekly cisplatin chemotherapy dosing versus triweekly chemotherapy with concurrent radiation for head and neck squamous cell carcinoma. Head Neck 41:2492–2499
Mohamed A, Twardy B, Zordok MA et al (2019) Concurrent chemoradiotherapy with weekly versus triweekly cisplatin in locally advanced squamous cell carcinoma of the head and neck: comparative analysis. Head Neck 41:1490–1498
Espeli V, Zucca E, Ghielmini M et al (2012) Weekly and 3‑weekly cisplatin concurrent with intensity-modulated radiotherapy in locally advanced head and neck squamous cell cancer. Oral Oncol 48:266–271
Tsan D‑L, Lin C‑Y, Kang C‑J et al (2012) The comparison between weekly and three-weekly cisplatin delivered concurrently with radiotherapy for patients with postoperative high-risk squamous cell carcinoma of the oral cavity. Radiat Oncol 7:215
Hesketh PJ, Grunberg SM, Gralla RJ et al (2003) The oral neurokinin‑1 antagonist aprepitant for the prevention of chemotherapy-induced nausea and vomiting: a multinational, randomized, double-blind, placebo-controlled trial in patients receiving high-dose cisplatin—the Aprepitant Protocol 052 Study Group. J Clin Oncol 21:4112–4119
Herrstedt J, Summers Y, Daugaard G et al (2018) Amisulpride in the prevention of nausea and vomiting induced by cisplatin-based chemotherapy: a dose-escalation study. Support Care Cancer 26:139–145
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
F. Weykamp, K. Seidensaal, S. Rieken, K. Green, S. Mende, K. Zaoui, K. Freier, S. Adeberg, J. Debus, and S.E. Welte declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Weykamp, F., Seidensaal, K., Rieken, S. et al. Age-dependent hemato- and nephrotoxicity in patients with head and neck cancer receiving chemoradiotherapy with weekly cisplatin. Strahlenther Onkol 196, 515–521 (2020). https://doi.org/10.1007/s00066-019-01550-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-019-01550-6